Table of Contents
Introduction
At times, patients visit the dentist with complaints of a severe burning sensation in their mouths. On examination, some of them are diagnosed with Oral Lichen Planus (OLP). However, many patients struggle to understand the nature of the disease progression in OLP. In this article, we’ll provide a simple, comprehensive overview of Oral Lichen Planus, its symptoms, causes, treatment, and natural remedies, along with some helpful dietary tips. We hope to make this information accessible to everyone, whether you’re a patient or just interested in learning more.
In this article, we will use the abbreviation “OLP” to refer to Oral Lichen Planus, so please keep that in mind as you read.
Presentation of Oral Lichen Planus
Oral Lichen Planus is a chronic inflammatory condition that can affect various parts of the oral cavity. A unique feature of OLP is that it follows a cyclical pattern, often described as waxing and waning. This means the disease flares up (waxing) for a few weeks, followed by a period of dormancy (waning), and then the cycle repeats.
Patients with OLP often experience episodes of burning sensations that come and go. The lesions can present in different forms, such as white lacy lines on a red background, which are often seen on the inner cheeks. However, OLP can also affect other areas of the mouth, including the gums, palate, and tongue.
Take the first step to a better Oral health!
Get tips on Oral health and discover ways to improve your Dental health. Sign up today
Note: Lichen planus can present in various forms and can sometimes be confusing to differentiate from other diseases. It is always recommended to consult an oral physician or an oral medicine expert for accurate diagnosis.
OLP on the Tongue
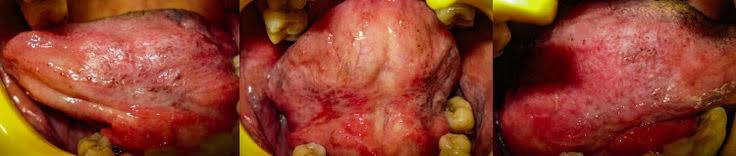
When OLP affects the tongue, it may result in depapillation, meaning a loss of taste buds in the affected area. White patches or white lines can also appear on the tongue, often accompanied by a severe burning sensation.
OLP on the Gums
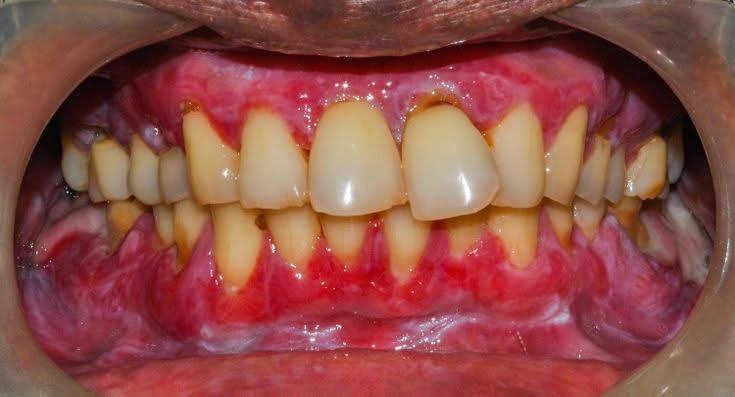
When OLP affects the gums, patients may experience severe swelling, pain, and inflamed gums that bleed easily. Diffuse white areas intermixed with red, inflamed gums are typical signs of OLP in this region.

A patient’s guide to Oral Lichen Planus
Did you know that only 2% of people with oral lichen planus (OLP) are at risk of developing oral cancer? Yet, finding complete and reliable information on OLP can be challenging. A Patient’s Guide to Oral Lichen Planus bridges that gap.
This comprehensive guide simplifies complex medical terms, offering clear, easy-to-understand information about managing OLP in daily life. Dr. Sai Kiran, with over a decade of experience in treating OLP, provides step-by-step advice on how to approach your dentist for treatment, along with current therapies—both conventional and alternative. Packed with practical tips and valuable resources, this book is the essential tool you need to take control of your OLP and improve your quality of life.
Don’t miss out on this authoritative guide—get your copy today!
Symptoms of Oral Lichen Planus
The hallmark symptom of OLP is a burning sensation, which is experienced by 90-95% of patients. This burning can make it difficult for patients to eat spicy foods, and in severe cases, the burning sensation can be felt even when drinking water.
Lesions often appear as white lines (reticular lichen planus) on a red, inflamed background. However, in some patients, there may be no white lines, only areas of redness and inflammation, especially in more severe forms such as Erosive Lichen Planus.
In some cases, the lesions may blister and rupture, causing profuse bleeding. This condition is known as Bullous OLP.
Learn more about Oral Leukoplakia: Symptoms, Causes, and Treatment
Causes of Oral Lichen Planus
The exact cause of OLP remains unclear, but it is believed to be related to an immune system dysfunction. Many experts consider OLP to be an autoimmune disease where the body’s immune cells mistakenly attack its own tissues, causing damage to the mucosal lining of the mouth.
Stress has also been identified as a significant trigger for OLP. Emotional stress, anxiety, and depression can exacerbate the condition and impact the effectiveness of treatment. Therefore, stress management is crucial for patients with OLP.
Biopsy for OLP Diagnosis
In some cases, the clinical presentation of OLP may not be as classic as described in textbooks, making it difficult to diagnose based solely on appearance. If there is any doubt, your dentist may recommend a biopsy to confirm the diagnosis histopathologically. The decision to undergo a biopsy should always be made by your dentist.
Treatment of Oral Lichen Planus
The main treatment focus for OLP is to alleviate the burning sensation that affects the majority of patients. Desensitizing mouthwashes or anesthetic rinses can provide temporary relief by reducing this discomfort, allowing patients to maintain adequate nutrition.
In addition to managing the burning sensation, treatment is aimed at reducing inflammation. Anti-inflammatory medications, such as corticosteroids, are commonly prescribed depending on the severity of the condition.
Stress management plays a crucial role in OLP treatment. Patients are encouraged to consult psychologists or stress therapists if needed. Nutritional supplements may also be recommended to support the healing process.
Oral Lichen Planus and Cancer Risk
While the probability of OLP transforming into oral cancer is low, it should not be ignored. A systematic review published in the Journal of Oral Disease reported a 1.37% chance of OLP becoming malignant. This transformation is more likely in cases of severe OLP with high levels of dysplasia (abnormal cell growth). Regular biopsy monitoring is essential to assess the stage of dysplasia and the risk of malignant transformation.
Diet for Oral Lichen Planus
Diet plays an essential role in managing OLP. A vegetarian diet rich in antioxidants can help promote healing. Foods like tomatoes, rich in lycopene, are beneficial for their antioxidant properties. Green tea, with its high flavonoid content, is also an excellent addition to the diet.
Additionally, foods rich in omega-3 fatty acids can help reduce inflammation and promote faster healing of oral lesions.
Managing stress is key to the natural treatment of OLP. Regular practice of yoga and meditation can help reduce stress and improve the effectiveness of medical treatments. Meditation has been shown to have a positive impact on OLP, working synergistically with medications.
Patients should also avoid foods or substances to which they are allergic, as these can aggravate OLP symptoms. A condition known as “Lichenoid Reaction” can mimic OLP but is triggered by allergies.
Explore more about the Best Toothpaste for Oral Lichen Planus
Frequently Asked Questions (FAQ)
Will OLP go away?
Unfortunately, OLP is a chronic condition with no cure. It only goes through periods of exacerbation (severe flare-ups) and remission (dormant phases).
Can OLP cause cancer?
Yes, OLP has a small potential to transform into oral cancer (squamous cell carcinoma), but the risk is low (1-2%).
Can OLP affect the throat?
Yes, OLP can cause symptoms similar to pharyngitis when it affects the throat.
Can OLP cause bad breath?
Yes, due to inflamed and swollen gums, OLP can lead to food retention and bad breath.
Does OLP cause dry mouth?
Dry mouth can be associated with OLP, especially due to medications used in its treatment.
Conclusion
Oral Lichen Planus (OLP) is a chronic condition with no definitive cure, but its symptoms can be managed with proper treatment, stress reduction, and dietary changes. Although it can cause significant discomfort, OLP does not generally pose a life-threatening risk. Regular dental visits, stress management, and adherence to treatment protocols are essential for maintaining oral health.
For more detailed information on oral health and OLP, consult with an oral medicine specialist. If you found this article helpful, please share it with your friends to raise awareness about this important condition.
Read more about OLP and other oral conditions at DentaDigest
- Is oral hygiene compulsory for kids? - January 13, 2023
- How to Choose the Best Dental Crown for Your Smile? - December 8, 2022
- Who needs antibiotics before dental work? What is antibiotic prophylaxis? - October 31, 2022




Pingback: The toothpaste you should avoid in lichen planus | DENTA DIGEST
Pingback: 10 things you should know about leukoplakia | DENTA DIGEST
I wish Dr Oz or Dr Phil had some PEOPLE on their show. So some people would know how bad this OLP IS. MENTALLY IT HAS DONE A NUMBER ON ME. MY HUSBAND EMAIL IS to ronald_dinsmore@yahoo.com. I don’t have one
Pingback: Oral Lichen Planus Cancer Symptoms | Dentadigest