People often misunderstand Oral lichen planus. They think that all lesions will finally lead to cancer. But the answer is “no”.
Oral Lichen planus is an inflammatory disease in the mouth, which might lead to a lot of discomfort to the suffering person.
Not all lesions might turn into Oral cancer. There is a probability of up to 2% in patients suffering from OLP, who might experience lesion turning into oral cancer.
Table of Contents
Take the first step to a better Oral health!
Get tips on Oral health and discover ways to improve your Dental health. Sign up today
Why do Oral lichen planus turn into cancer?
Every lesion in OLP might not turn into Oral cancer in every patient. There are some predisposing factors added to genetic susceptibility, for determining whether a person might develop or has developed Oral cancer.
Oral lichen planus itself might never turn into Oral cancer unless it is provoked by other confounding factors. Here is a list of factors that might aggravate the process of conversion of OLP into Oral cancer.
- People with smoking habits are more susceptible to developing Oral cancer in OLP.
- Chronic alcoholics might have high probability of developing Oral cancer in OLP patients.
- Patients with uncontrolled diabeties and recurrent candidal infection in the mouth might develop Oral cancer.
- Patients with suseptible genes for cancer might develope Oral cancer from OLP at a faster pace.
- Chronic irritation in the region of OLP due to root stumps or sharp teeth might lead to long standing ulcers which might later develop into oral cancer.
In most patients, OLP is a regular lesion that might cause some discomfort like burning sensation and pain in the mouth. But in very few, it might turn into a harmful lesion and might lead to Oral cancer.
How do I identify Oral lichen planus cancer symptoms ?
Here are a few symptoms you should identify in an Oral lichen planus lesion turning into oral cancer.
Persistent ulcer
Long-standing persistent ulcers which are not healing are a sign of Oral cancer changes. Ulcers in patients with oral lichen planus usually heal within a few days or when once the remission of the lesion starts.
But in patients who are developing oral cancer, these ulcers remain persistent and will not heal. The ulcers become painless and hard in consistency.

Growth
Growth in and around the OLP lesion might be a sign of Oral cancer. We might see a proliferative growth in the involved region which might be painless unless infected with a secondary infection.
The region in and around the growth becomes hard.
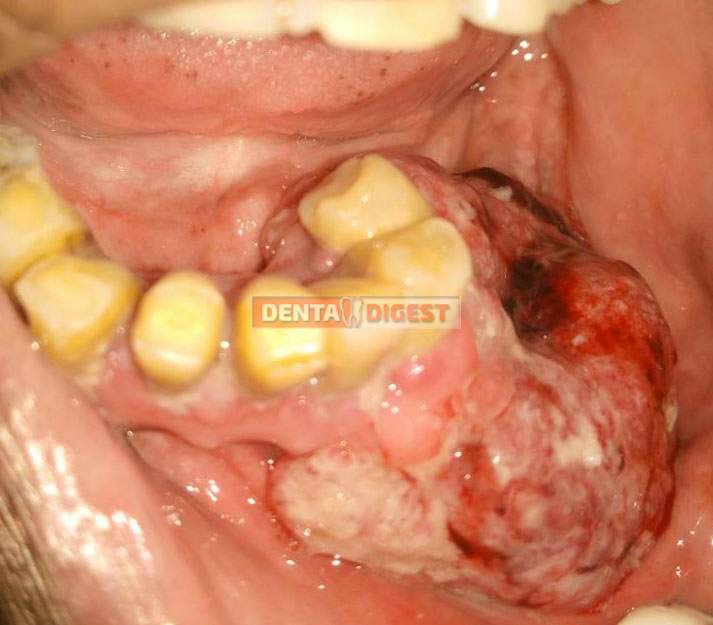
Thick skin with increased redness
Oral cancer develops with the development of a condition called dysplasia in the cells. Hence as the dysplasia increases at the cellular level, the tissues become more leathery and tough.
As a result, the skin inside the mouth becomes hard and leathery inconsistency. Such patients might experience an increased burning sensation.
Moreover, the lesion appears bright red in color and often bleeds on mild trauma.
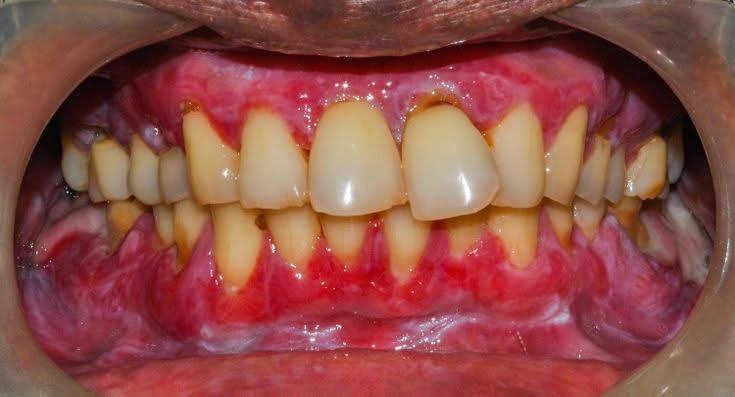
How to diagnose developing oral cancer in Oral lichen planus patients?
People often panic when they observed some change in their oral cavity or mouth. But one thing should be remembered.
Lichen planus turning into oral cancer is rare. There are a lot of factors that influence OLP turning into Oral cancer. Hence my advice is “Every change you see in your mouth might not be related to Oral cancer”.
Biopsy
In case of doubt, you can always visit your dentist and have a biopsy done for diagnosis. Do not jump to conclusions, as OLP is treatable.
A biopsy is a gold standard for OLP diagnosis. It is always better to have a second opinion on your histopathological report in case you still have a doubt about the lesion.
Can I prevent Oral cancer from developing from Oral lichen planus?
Yes! to some extent. You can follow these guidelines to have a safe healing process during the stages of exacerbation in Oral lichen planus.
Healthy diet
Have good food. A healthy diet helps in healing the skin inside the mouth. As a result, the OLP lesions heal faster and will not irritate the mouth for longer periods.
Foods, rich in omega-3 fatty acids aid in faster healing and provide relief from burning sensations. Lesser irritation has fewer chances of the lesion turning into Oral cancer.
Sharp teeth
Sharp teeth often irritate the skin around the teeth. It might result in traumatic ulcers which might later turn into Oral cancer.
Hence always have your sharp teeth trimmed. Tooth surfaces with smooth cusps aid in reducing friction between teeth and the skin within the mouth.
Control blood glucose levels
High and uncontrolled blood glucose levels might often cause severe candidal infections in the mouth. Such presentation should be stopped as a prolonged candidal infection inside the mouth might lead to Oral cancer.
In simple words, the candidal infection might hasten the process of Oral cancer development in these patients.
Good oral hygiene
Good oral hygiene is vital for your overall health. Studies say that patients with poor oral hygiene have elevated symptoms of burning sensation and other presentations in OLP.
Hence, dentists often advise patients with OLP to undergo teeth cleaning and polishing regularly. It aids in the maintenance of good oral hygiene and also reduces the severity of symptoms.
Get away from irritants
Recently, I have seen an article in a blog regarding baking soda wash for treating lichen planus. I was shocked. How can people be so dumb to use an irritant to clean or treat OLP?
My sincere advice to all readers is that there is plenty of nonsense available on the net. Be cautious and selective while following.
Baking soda might cause or increase the severity of oral lichen planus, as it irritates the mucosa or skin in the mouth. If you find something more irritating in the mouth, my advice is to stop using it as it might aggravate OLP.
Some toothpaste that contains clove and other acidic materials might cause an increase in burning sensation. Such patients should avoid using these pastes.
Also read:
Regular check-up
Visit your dentist regularly and have check-ups done. Regular monitoring of the condition of Oral lichen planus, in your mouth, is vital for properly managing the disease.
Any change in the lesion type or character might drag the attention of your dentist in time. It can be confirmed by a diagnosis that prevents further complications.
- Is oral hygiene compulsory for kids? - January 13, 2023
- How to Choose the Best Dental Crown for Your Smile? - December 8, 2022
- Who needs antibiotics before dental work? What is antibiotic prophylaxis? - October 31, 2022


