Table of Contents
Overview
Doctor! Do I get an infection after a root canal? What are the signs of infection after a root canal? It is one of the most common questions that my patients ask before a root canal procedure.
If you are one of them, then you are in the right place. Yes! Root canal treated teeth do get infected. Here are few signs through which we can identify an infected root canal treated teeth.
Although it is rare, it is not impossible for a root canal treated teeth to be infected. The severity of infection might range from a small pain to severe swelling.
Every patient needs to be aware and identify the symptoms as early as possible to prevent complete loss of teeth. Moreover, early intervention can increase the lifespan of the root canal tooth.
Take the first step to a better Oral health!
Get tips on Oral health and discover ways to improve your Dental health. Sign up today
Causes of infection after a root canal
What causes infection in a root canal treated teeth? The answer to this question is multifactorial. Here are a few common reasons for infection after a root canal.
Incomplete root canal

Failure to complete the root canal procedure might be one of the reasons for a secondary infection. It could be the patient’s sheer irresponsibility in attending the complete treatment or might be the doctor’s negligence in completing the root canal.
Every root canal procedure ends with a successful filling of the canal with an inert material called gutta-percha. This procedure is called obturation. If the obturation is incomplete, then the canal provides ample space for bacteria to re-grow and re-infect the root canal.
Pain from teeth usually subsides on the first day of the root canal treatment itself. In such conditions, few patients might neglect to revisit the dentist. It leads to an incomplete root canal procedure.
Chronic infection leading to root resorption
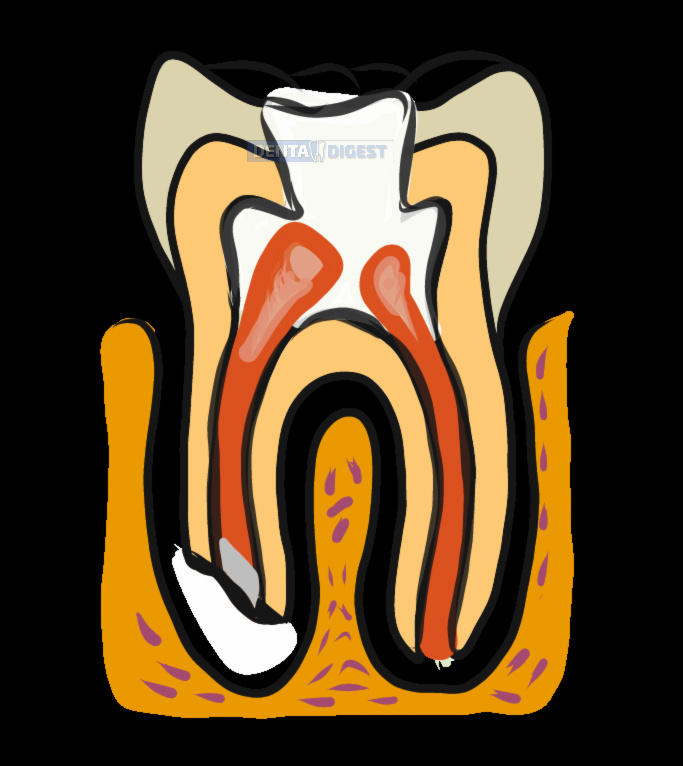
Teeth with the disease produce chronic abscesses below the root. In a few conditions, the abscess can induce root resorption. In simple words, the pus accumulated below roots can degrade the root causing root resorption.
Such root resorptions are not ideal for root canal treatments. Treatment in such teeth might lead to re-infection.
Fractured root

Each tooth contains a vital region called pulp in the center of the teeth. The essential area includes nerves and blood vessels.
When a tooth gets infected to its core, the vital region becomes decomposed or destroyed. At the same time, the teeth become dry and brittle.
When a root canal procedure is done in such teeth, there are ample chances for the root to be fractured. The fractures in the root during the treatment are difficult to diagnose. But patients often complain of severe pain in their teeth after root canal procedures.
Teeth with a fracture in a canal are not ideal for root canal treatment. If such teeth are treated with root canal procedures, there are ample chances for the teeth to get re-infection.
Delayed crowning
What is the ideal time to place a crown over the teeth? Is it immediately after the root canal procedure?
It is a familiar doubt everyone gets after their root canal treatment. The answer to this question varies from doctor to doctor.
Some dentists prefer immediate crowning after the root canal procedure, while others prefer waiting for some time.
We usually prefer to wait at least for a week after the root canal procedure. This gives ample time for the dentist to observe how teeth are responding to root canal treatment. If everything goes well, we advise patients to go for a crown after one week.
But, a few patients might miss the appointments after one week. This could turn out to be challenging for the patients and dentists.
Root canal-treated teeth lack nutrient supply. As a result, the teeth become non-vital and brittle. Such teeth cannot bear extreme stress and often get chipped off. A crown in such conditions can act as a protective layer around the teeth.
Root canal-treated teeth without a crown can break during eating. It can lead to re-infection.
What is the right time to crown teeth after a root canal procedure?
Root abnormalities (accessory canals, curved roots)
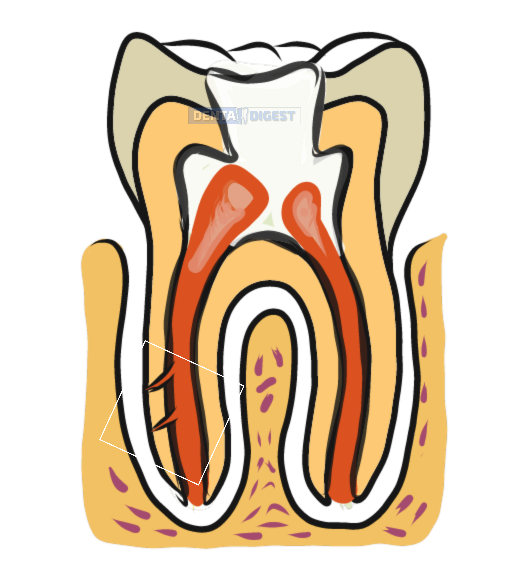
Depending on the type of teeth, the number of root canals ranges from one to three. Few teeth might have extra canals.
In addition to it, a few teeth might have tiny canals around the central canal called accessory canals.
The accessory canals are difficult to identify in regular radiographs. Hence dentists might overlook them during root canal procedures. Such treatments lead to severe pain after the root canal procedure.
Few teeth have abnormal root morphology. A deep curve in the root is difficult to treat. Such canals are called dilacerated canals.
Dentists often struggle in obturating them. It can lead to incomplete root canal treatment.
Five signs of infection after a root canal
Re-infection of a root canal should be identified at an early stage. Here are five vital signs which indicate re-infection in your teeth.
Persistent pain
Pain is a common symptom in patients with deep caries. The pain usually subsides after root canal treatment. Few patients might sense mild discomfort for a week, even after a root canal.
But, persistent, severe pain even after a root canal procedure is a sign of root canal failure or infection in root canal-treated teeth.
Pain after the root canal. How to manage.
Pimple-like structures on gums
Few patients might find a pimple-like structure on the gums, right above the root canal-treated teeth. It is a blister containing pus. Such a presentation is a sign of re-infection.
Such a condition is called a dentoalveolar abscess, which might arise if the root canal procedure is not done in aseptic conditions.
Gum swellings
Some patients often experience severe gum swelling after the root canal procedure. Such engorgement could be from a re-infected root canal.
Mobile teeth
An increase in the mobility of teeth after the root canal is a sign of root canal failure. If a patient experiences increased mobility of treated teeth, the possible reason could be a secondary periodontal infection.
In simple words, the root canal-treated teeth get re-infected. The infection from the root canal enters into the surrounding supporting structure of teeth, which is called the periodontium. It results in increased mobility of teeth.
Fever
Infection from teeth can spread into the blood. Such a condition is called septicemia. If the infection does not subside in root canal-treated teeth, it has an excellent chance to enter the primary bloodstream.
Patients with a fever after a root canal procedure might experience such septicemia conditions. It is a sign of patent infection in root canal-treated teeth.
Treatment options
Medication
Some infections do reside after root canal treatment. It is called a residual infection. It has to be cleared by our body’s immune system. This is the reason why patients suffer from mild pain even after root canal treatment.
But this pain is of mild intensity and will be relieved within a span of 1 week or ten days. The healing process can be accelerated by using a few painkillers.
If pain persists even after medication, then opt for the next treatment options.
Second root canal
Severe pain after a root canal procedure might be a sign of root canal infection. In such conditions, your dentist might opt for a re-root canal procedure or a second root canal procedure.
Apicoectomy
A persistent abscess associated with root resorption might cause root canal failure. Such teeth require apicoectomy. It is a procedure where the apex of the infected root is removed and closed with a restorative material.
Extraction
If no treatment produces relief from pain, the last treatment option might be extraction or teeth removal.
Preserving the natural teeth is vital as no alternative fits precisely into its place.
FAQs
Are root canals painful?
No, the procedure is performed under local anesthesia. Hence root canals are not painful.
However, in case of severe infections, the local anesthesia might not work properly and may cause some disturbance in the initial stage of the procedure.
Are root canal safe?
Yes, root canals are completely safe. Of course, there has been some information roaming in the net regarding the safety of root canals, but there is no scientific proof stating that root canals might harm you.
Are root canals dangerous?
Root canal therapy is typically regarded as a safe and common dental procedure. They are used to treat and save a badly diseased or decaying tooth. While there are hazards with any medical operation, the risks of root canals are quite minor when compared to the risks of leaving an infected tooth untreated.
Are root canal teeth dead?
yes! Root canal teeth are dead teeth devoid of any blood and nutritional supply.
Can a root canal cause cancer?
The idea that root canals cause cancer is not supported by scientific data. This concept is based on the disputed and outmoded “focal infection theory,” which contends that chronic infections in the mouth, even root canal-treated teeth, can rise to systemic disorders such as cancer. However, the scientific world has overwhelmingly dismissed this notion.
Can root canals get infected?
Yes! Root canals often get infected if not maintained properly. Continuous food lodgment and seepage of fluids into the teeth treated for root canal might cause secondary root canal infection.
Can root canal infection spread?
Yes, untreated root canal infections might spread into surrounding tissue spaces and result in a larger and worse space infection.
Can root canal pain come and go?
Yes, people often complain of periodic pain in root canal infections. People usually complain of severe pain when the opening of the pulp is blocked by food or other debris and get relief from the pain after unblocking it.
Can a root canal be done through the crown?
Yes! It can be done through Crown but needs expertise.
Can the root canal be redone?
Yes! In case of consistent pain, the root canal procedure can be repeated by removing the old obturation in the canal. The entire procedure is called the Re-root canal or Re-RCT.
Can a root canal cause tinnitus?
Tooth infection, specifically the upper wisdom teeth infection might spread into the middle ear to cause tinnitus. But root canals might not cause any middle ear infections or tinnitus.
Can a root canal cause trigeminal neuralgia?
No!
What root canal cement is economically used?
Zinco oxide eugenol cement is most commonly used in root canals. Glass ionomer cement is usually used to close the root canals.
Composites are the premium options for filling a root canal-treated tooth.
When the root canal is needed?
When the pulp, the soft tissue inside the tooth, becomes infected or injured, a root canal is required. Deep tooth decay, a broken tooth, repeated dental operations on the same tooth, or trauma to the tooth can all cause the pulp to become infected.
When a root canal doesn’t work?
In cases like chronic infections where the infection spreads beyond bone and is associated with severe bone loss, usually, root canals might not be the best option in such cases.
Read more
- What are the signs of a root canal?
- How much does a root canal cost?
- Does a root canal cause cancer?
- Crown after root canal
- Pain after a root canal?
- Is oral hygiene compulsory for kids? - January 13, 2023
- How to Choose the Best Dental Crown for Your Smile? - December 8, 2022
- Who needs antibiotics before dental work? What is antibiotic prophylaxis? - October 31, 2022




Pingback: Best root canal tips you should know before treatment | DENTA DIGEST
Thanks for sharing this informative blog.I hope people should get an idea on whether they should go with Invisalign or not.
Pingback: WISDOM TOOTH INFECTION. A PATIENT’S GUIDE TO MANAGE PERICORONITIS | Dentadigest